Karen Jenkins, a 55-year-old Navy veteran, had always been proactive about her health. She exercised regularly, ate a balanced diet, and visited her doctor for annual check-ups. So, when she woke up one morning with severe chest pain, she knew something was wrong. Jenkins immediately drove herself to the emergency room, convinced she was having a heart attack.
“I was sweating, my heart was racing, and I couldn’t catch my breath,” Jenkins recalled. “I’ve never experienced anything like it before. I just knew I needed to get to the hospital as quickly as possible.”
Upon arrival, Jenkins was quickly ushered into a treatment room where a team of doctors and nurses began assessing her condition. They took her vitals, ran an electrocardiogram (ECG), and performed a series of tests to determine the cause of her symptoms.
Initially, doctors suspected a heart attack, given Jenkins’ symptoms and medical history. However, as the test results began to roll in, they revealed a surprising diagnosis.
“Karen, your ECG and blood work are all coming back normal,” said Dr. Thompson, Jenkins’ attending physician. “Your heart appears to be functioning normally, but we did find something else that’s causing your symptoms.”
Jenkins was confused and concerned. “What could it be?” she asked.
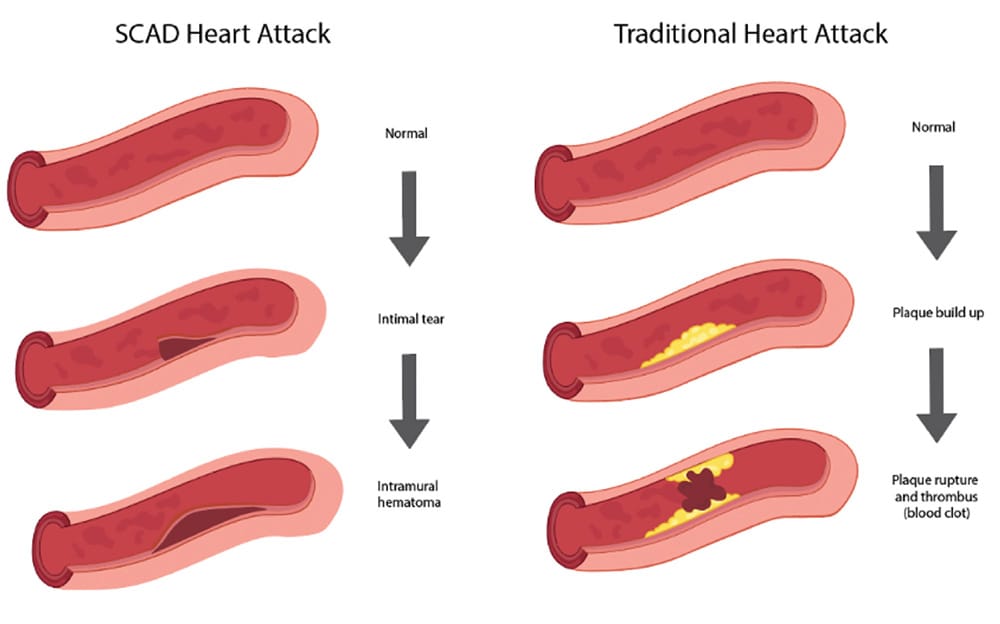
Dr. Thompson explained that Jenkins had a rare condition known as Spontaneous Coronary Artery Dissection (SCAD). SCAD occurs when there is a tear in one of the blood vessels in the heart, causing a blockage that can lead to a heart attack.
However, in Jenkins’ case, the tear was not causing a blockage, but rather a constriction of the blood vessel, which was leading to her symptoms.
“We’re going to need to perform an angiogram to confirm the diagnosis and determine the best course of treatment,” Dr. Thompson explained.
Jenkins was taken to the catheterization lab where a team of doctors and nurses performed the angiogram. The test confirmed the diagnosis of SCAD and revealed that Jenkins had a 90% constriction of the affected blood vessel.
“We’re going to need to insert a stent to open up the blood vessel and restore blood flow to the heart,” said Dr. Lee, the interventional cardiologist.
Jenkins was taken to the operating room where the stent was successfully inserted. The procedure was a success, and Jenkins began to feel relief from her symptoms almost immediately.
“I couldn’t believe it,” Jenkins said. “I was expecting to have a heart attack, and instead, I had this rare condition that I had never heard of before.”
Jenkins spent several days in the hospital recovering from the procedure. She was prescribed medication to manage her symptoms and prevent future episodes.
“It’s been a few months since the diagnosis, and I’m feeling much better,” Jenkins said. “I’ve had to make some lifestyle changes, but I’m grateful to have received the care I needed when I needed it.”
Jenkins’ experience highlights the importance of seeking medical attention immediately if symptoms persist or worsen over time. It also underscores the need for doctors to consider rare conditions in their diagnoses.
“SCAD is a rare condition, but it’s not unheard of,” said Dr. Thompson. “As doctors, we need to stay vigilant and consider all possibilities when diagnosing patients.”
Jenkins’ journey has also raised awareness about the importance of women’s heart health. According to the American Heart Association, heart disease is the leading cause of death among women in the United States.
“Women often ignore their symptoms or attribute them to other conditions,” said Dr. Lee. “It’s essential for women to be proactive about their heart health and seek medical attention if they experience any symptoms.”
Jenkins’ experience has been a wake-up call for her and her family. They have all become more aware of the importance of heart health and the need to seek medical attention immediately if symptoms persist.
“I’m just grateful to be alive,” Jenkins said. “I hope my story can raise awareness and help others who may be experiencing similar symptoms.”