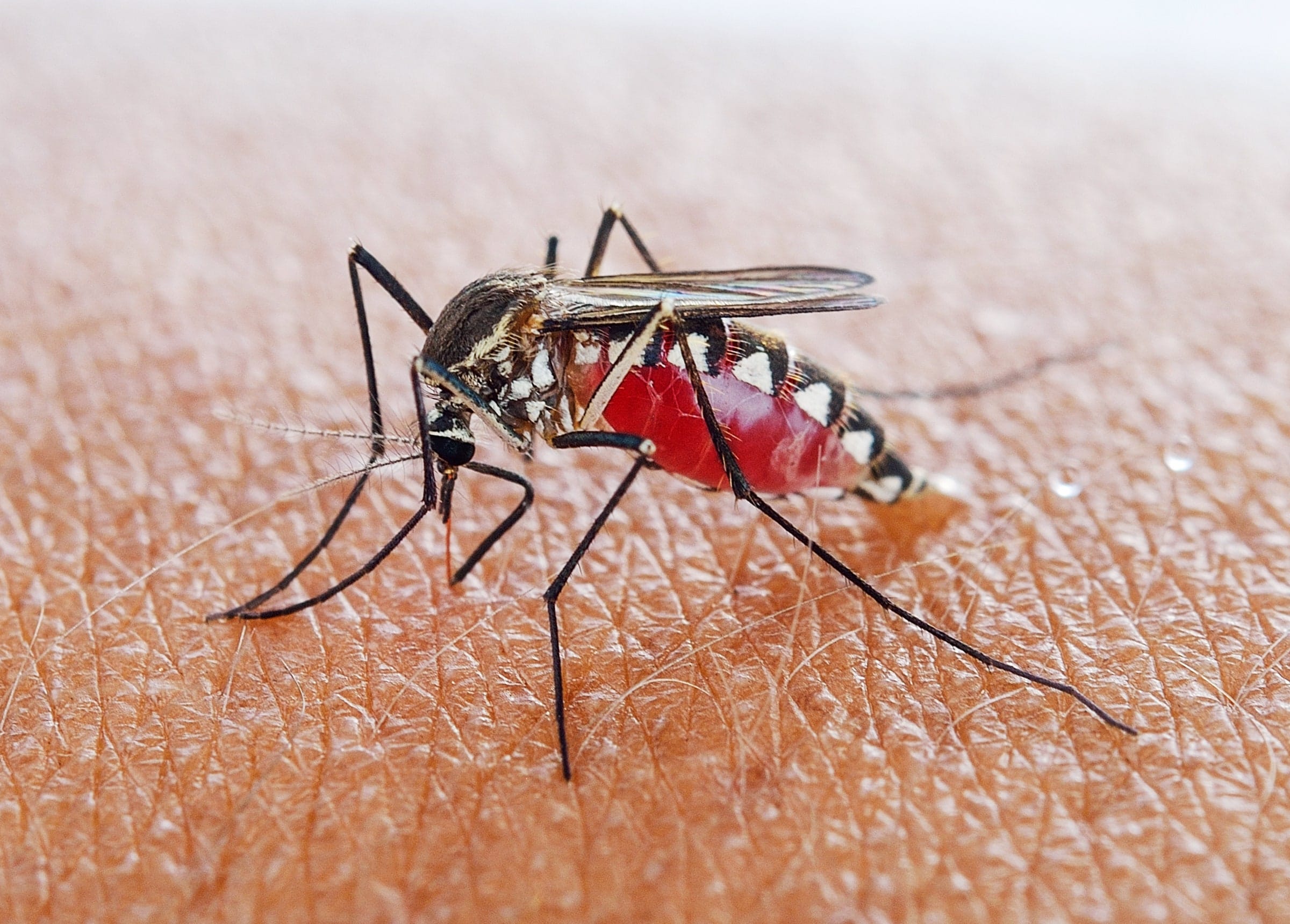
Malaria, a mosquito-borne disease caused by Plasmodium parasites, continues to pose a substantial threat to global health, particularly in sub-Saharan Africa, Southeast Asia, and parts of South America. While considerable progress has been made in combating the disease in past decades through insecticide-treated bed nets, improved diagnostics, and effective antimalarial drugs, recent data indicates a worrying resurgence in cases and fatalities. This resurgence underscores the complex nature of the disease and the need for ongoing vigilance, innovation, and a coordinated, multi-pronged approach to ensure effective control and eventual elimination.
The World Health Organization (WHO) reports that after years of decline, malaria cases and deaths have plateaued and are showing signs of increasing in certain areas. Factors contributing to this concerning trend include insecticide resistance in mosquito populations, drug resistance in malaria parasites, and disruptions to essential health services due to conflicts, natural disasters, and, most recently, the COVID-19 pandemic. Climate change is also playing an increasingly significant role, altering vector ecology and distribution, thus expanding the geographical range of malaria transmission.
The rise in insecticide resistance is particularly alarming. Pyrethroids, the most commonly used class of insecticides in treated bed nets and indoor residual spraying, are becoming less effective in many regions. This means that the primary method of preventing mosquito bites, a cornerstone of malaria control efforts, is being compromised. Similarly, antimalarial drugs, such as artemisinin-based combination therapies (ACTs), which have been highly effective in recent years, are showing signs of resistance, especially in parts of Southeast Asia. This resistance can lead to longer treatment durations, increased hospitalization rates, and higher mortality, posing a grave threat to the gains made over the last two decades.
The COVID-19 pandemic has further complicated the situation. Lockdowns and disruptions to health systems have hindered access to testing, treatment, and preventive measures, resulting in a rise in untreated malaria cases. This has led to increased mortality, particularly among vulnerable populations such as children under five and pregnant women. The pandemic has also diverted resources and attention away from malaria control efforts, causing further setbacks.
Addressing the current malaria situation requires a renewed commitment to international collaboration and resource allocation. National governments, international organizations, and private foundations need to work together to implement a comprehensive set of strategies that target all aspects of malaria transmission and treatment. This approach must include:
Strengthening surveillance systems: Reliable data is essential for tracking malaria cases, identifying emerging outbreaks, and monitoring drug and insecticide resistance patterns. Investing in enhanced surveillance capabilities, including molecular diagnostics and rapid reporting systems, can facilitate timely responses and prevent widespread transmission.
Developing new tools and technologies: Research and development of new insecticides with different modes of action and new antimalarial drugs that are effective against resistant parasites are critical. New diagnostic tools are also needed that are faster, more accurate, and can be used in resource-limited settings. The development of an effective malaria vaccine is also a crucial priority and would revolutionize malaria prevention efforts.
Scaling up existing interventions: Ensuring universal access to insecticide-treated bed nets, indoor residual spraying, prompt diagnosis, and effective treatment with ACTs remains paramount. Targeted interventions should be implemented to reach vulnerable populations, particularly in remote or hard-to-reach areas. Community health workers play a vital role in distributing bed nets, providing rapid testing, and administering treatment in remote locations, therefore their importance shouldn’t be understated.
Engaging communities: Educating communities about malaria prevention and treatment is crucial for promoting health-seeking behaviors and encouraging the proper use of preventive measures. Community involvement in malaria control programs helps build trust, ensures cultural appropriateness, and increases program acceptance.
Addressing social determinants of health: Factors such as poverty, malnutrition, lack of access to clean water and sanitation, and inadequate housing conditions increase vulnerability to malaria. Therefore, addressing these underlying social determinants is essential for long-term malaria control and elimination. Poverty reduction, improved sanitation, and access to quality healthcare can make significant contributions to improving community health and resilience.
Investing in health system strengthening: Malaria control efforts must be integrated into broader health system strengthening initiatives. This includes investing in training healthcare workers, upgrading infrastructure, ensuring a reliable supply of essential commodities, and building sustainable health systems that can respond effectively to future health threats.
Climate change mitigation and adaptation: Considering the growing link between climate change and malaria transmission, implementing climate-sensitive control measures and mitigating the effects of climate change is crucial. This includes incorporating climate data into malaria risk mapping, adapting control strategies to changing environmental conditions, and promoting sustainable development that reduces human impact on the environment.
The global community must acknowledge that the fight against malaria is far from over. The recent setbacks demonstrate the need for sustained effort and commitment. Increased funding for malaria control and research is essential, as is fostering partnerships between the public and private sectors to drive innovation and resource mobilization.
Additionally, it is vital to maintain a robust global research agenda focused on understanding parasite and vector biology, drug and insecticide resistance mechanisms, and identifying new targets for intervention. This requires building capacity in low- and middle-income countries to conduct research and develop context-appropriate solutions. Data analysis and information sharing are equally important in order to inform control programs.
International collaborations should focus on building consensus around best practices and strengthening coordination mechanisms. This involves engaging a variety of stakeholders, such as governments, international organizations, non-governmental organizations, research institutions, and the private sector. Aligning resources and efforts can help avoid duplication and maximize impact, fostering a united front against malaria.
Furthermore, monitoring progress regularly is crucial. This involves using surveillance data to track the effectiveness of interventions, identify gaps in implementation, and adjust strategies accordingly. Regular program evaluations are needed to ensure that resources are being used efficiently and that programs are achieving their intended goals.
The malaria situation calls for a renewed focus and sustained effort. By working together, nations can revitalize the battle against this devastating disease. This concerted effort must include a comprehensive, multi-faceted approach, which incorporates research, innovation, community engagement, capacity-building, and a renewed commitment to global health.
The road ahead may be challenging, but with sustained dedication, collaboration, and investment, we can ensure a future where no one dies from malaria.